Schedule An Appointment With Us
Are Your Symptoms Affecting Your Quality Of Life?
Consult our MOH-accredited orthopaedic surgeon for an accurate diagnosis & personalised treatment plan.
MBBS
MRCSEd
MMED (Ortho)
FRCSEd
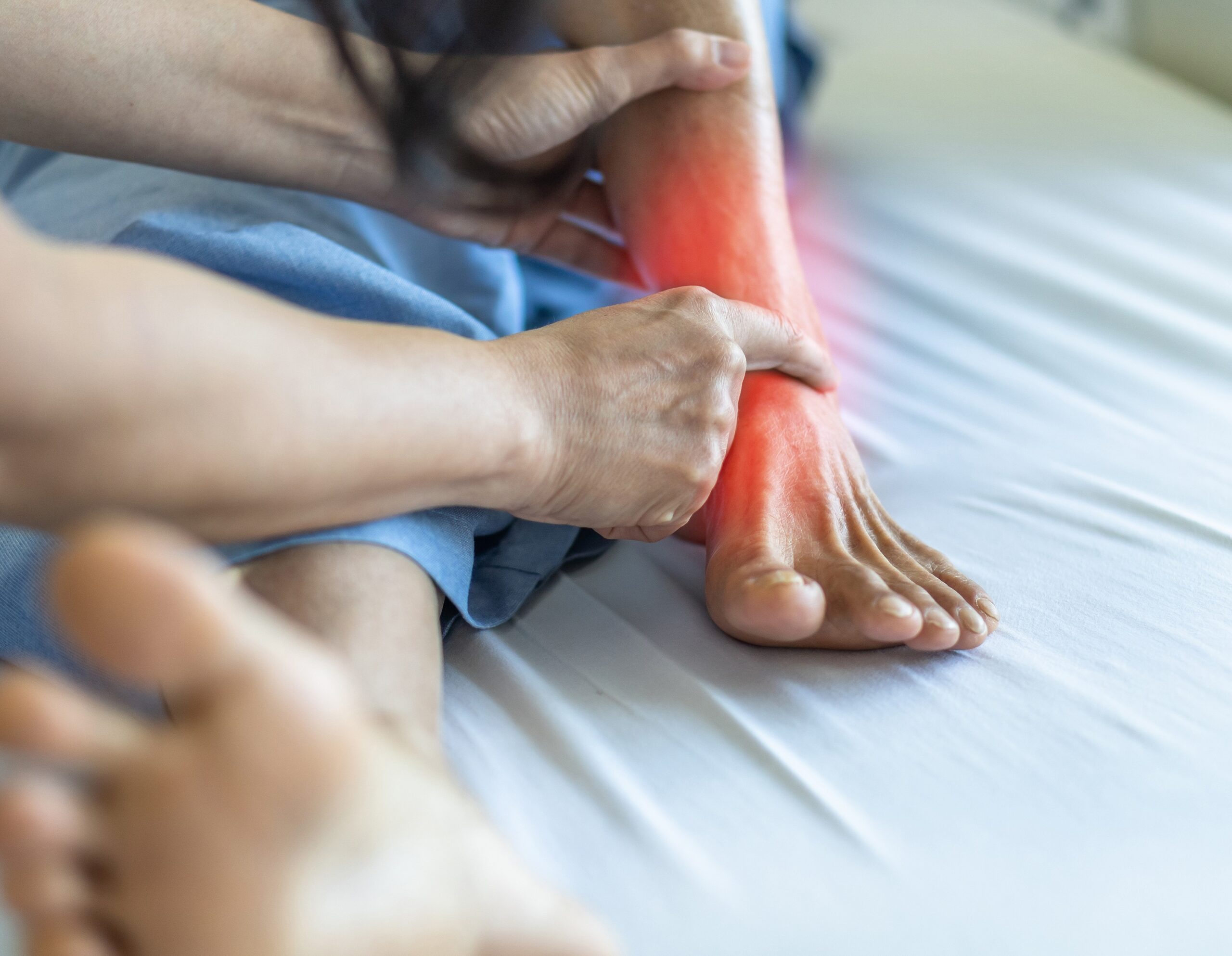
Posterior tibial tendon dysfunction (PTTD) is a condition where the posterior tibial tendon becomes inflamed or damaged. This tendon connects the calf muscle to the bones on the inside of the foot and plays a role in supporting the foot’s arch. In PTTD, the compromised tendon may lead to a progressive flattening of the foot, commonly referred to as adult flatfoot.
This condition is characterised by the posterior tibial tendon’s inability to provide adequate support and stability for the foot’s arch, leading to a gradual collapse of the arch. The progression of PTTD can lead to changes in foot alignment, impacting mobility and overall foot function.
PTTD can arise from a variety of causes, often involving a combination of intrinsic and extrinsic factors.
PTTD presents a range of symptoms and signs, which usually progress as the condition worsens.
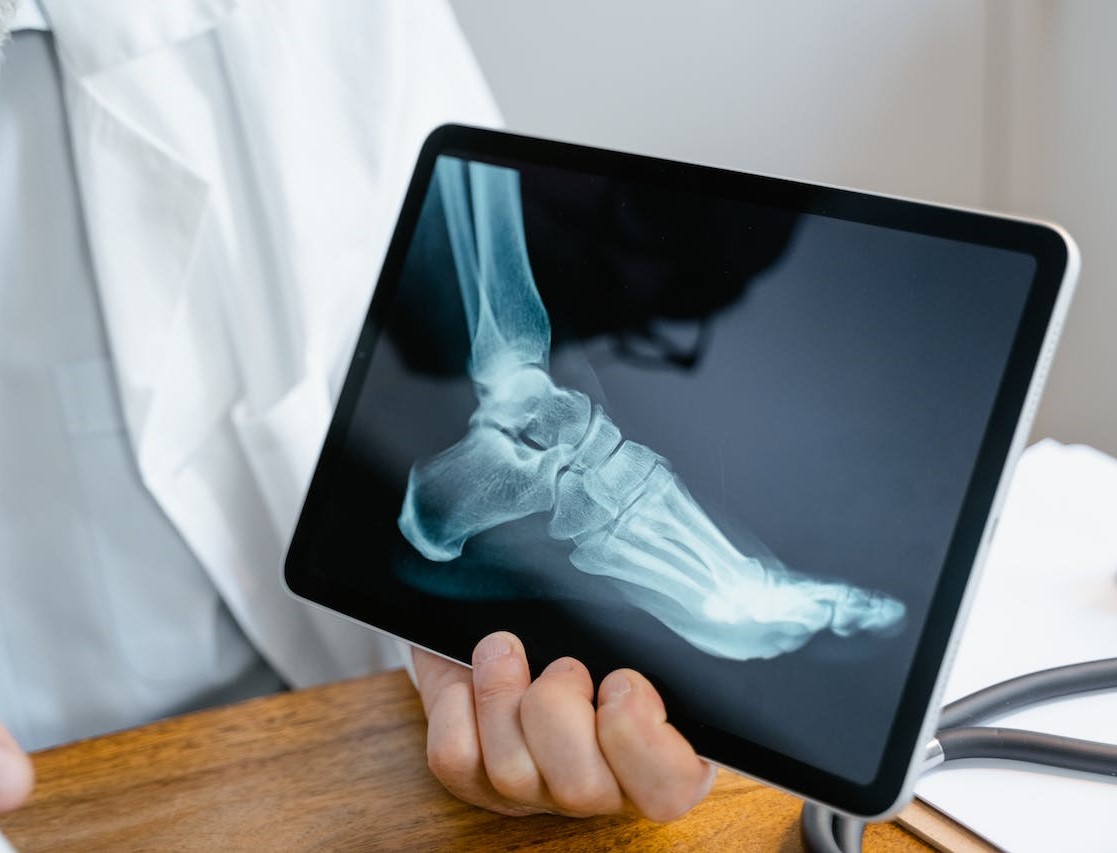
Diagnosing PTTD involves a combination of medical history review, physical examination, and diagnostic imaging.
Non-surgical treatment methods are often the first line of approach for PTTD, especially in the early stages of the condition. These strategies aim to alleviate symptoms and prevent further deterioration of the tendon.
Rest and Activity Modification |
For less serious cases, the foot and ankle specialist may initially suggest reducing or ceasing activities that aggravate the symptoms. Patients should avoid high-impact activities and instead engage in low-impact exercises like swimming or cycling. |
Nonsteroidal Anti-inflammatory Medications (NSAIDs) |
Over-the-counter medications such as ibuprofen or naproxen can help manage pain and inflammation. |
Use of Orthotic Devices |
Custom shoe inserts or braces may be used to provide support for the arch and alleviate stress on the posterior tibial tendon. |
Physical Therapy |
Physical therapy can help maintain joint flexibility and muscle strength. This may include exercises to strengthen the posterior tibial tendon and improve foot and ankle mobility. |
When non-surgical treatments for PTTD do not yield sufficient improvement, or if the condition is in a more advanced stage, surgical intervention may be necessary. The choice of surgery depends on the severity and specific characteristics of the patient’s condition.
This procedure involves lengthening the calf muscles (specifically the gastrocnemius muscle). It aims to improve ankle movement and reduce the stress on the posterior tibial tendon. Gastrocnemius recession is often considered when tight calf muscles contribute to the patient’s condition.
In this procedure, the foot and ankle specialist removes the inflamed tissue surrounding the posterior tibial tendon (tenosynovium). Tenosynovectomy is beneficial in reducing pain and swelling and is often performed in conjunction with other procedures to address tendon damage.
This involves rerouting another tendon from the foot to replace or assist the function of the damaged posterior tibial tendon. A tendon transfer is used to restore the strength and stability of the foot, particularly in cases where the posterior tibial tendon is severely damaged or torn.
In cases of severe deformity, an osteotomy, which involves cutting and shifting the bones of the hindfoot, may be performed to recreate the arch of the foot.
For patients with severe arthritis, fusion of the affected foot joints may be necessary. This involves removing damaged cartilage and bone and fixing the bones together to reduce pain and improve stability.
Schedule An Appointment With Us
Consult our MOH-accredited orthopaedic surgeon for an accurate diagnosis & personalised treatment plan.
While PTTD cannot always be completely prevented, several strategies can reduce the risk of developing the condition.

MBBS
MRCSEd
MMED (Ortho)
FRCSEd
With over 18 years of experience, Dr Poh Seng Yew is an orthopaedic surgeon specialising in hip, knee, shoulder and elbow surgery, sports medicine, and trauma surgery.




Weekdays: 9.00am – 5.00pm
Saturdays: 9.00am – 1.00pm
Sundays and Public Holidays: Closed
Please leave us a message, and we will be in touch with you shortly.
PTTD progresses through four stages, ranging from mild to severe. Stage I involves injury to the tendon without tearing, Stage II involves a torn or dysfunctional tendon with foot deformity, Stage III is marked by severe foot deformity and degenerative changes in connective tissue, and Stage IV includes degenerative changes in the ankle joint.
The healing time for PTTD varies based on the severity and treatment approach. Early-stage PTTD may respond well to non-surgical treatments within weeks to months, whereas more advanced stages requiring surgery might necessitate a longer recovery period.
Walking with PTTD is possible, but it may be challenging, especially in advanced stages. Using supportive footwear and orthotic devices can help alleviate discomfort. If walking causes severe pain, seek guidance from a foot and ankle specialist for appropriate management strategies.
Untreated PTTD can lead to worsening symptoms, increased pain, and further foot deformity. Progressive stages of PTTD can impact mobility and quality of life. Timely consultation with a foot and ankle specialist can help manage the condition and reduce the risk of long-term complications.