Schedule An Appointment With Us
Are Your Symptoms Affecting Your Quality Of Life?
Consult our MOH-accredited orthopaedic surgeon for an accurate diagnosis & personalised treatment plan.
MBBS
MRCSEd
MMED (Ortho)
FRCSEd

Adult flatfoot, also known as adult-acquired flatfoot deformity (AAFD), is a condition characterised by the flattening of the arch in one or both feet. This is often accompanied by the foot turning outward. It results from various foot problems and can alter the alignment of the legs, potentially affecting the ankles and knees.
The lack of proper arch support in the foot can lead to overpronation, placing excess strain on the ankles and potentially leading to additional conditions like ankle instability and tendonitis.
Adult flatfoot can stem from several factors, each contributing to the weakening or alteration of the foot’s structure.
The manifestation of adult flatfoot can vary, with several symptoms indicating the presence of this condition.
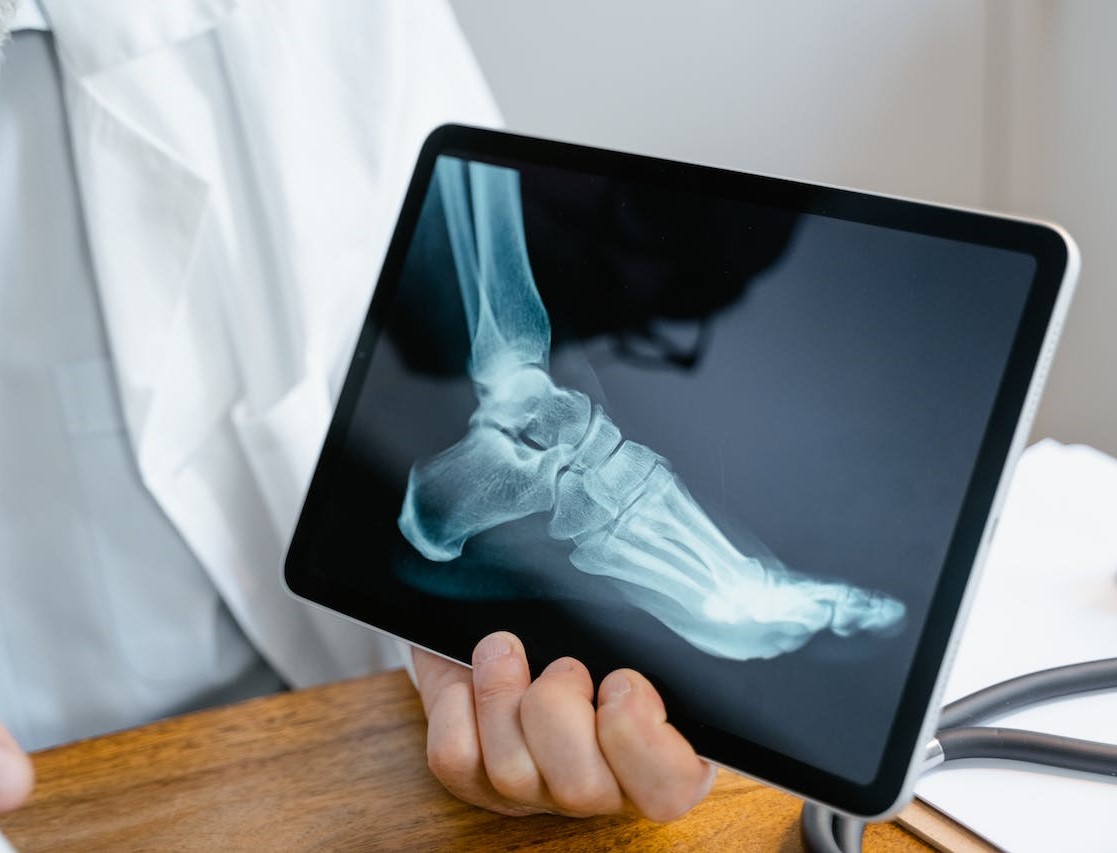
The process of diagnosing adult flatfoot involves a combination of physical examination, imaging techniques, and medical review.
Addressing adult flatfoot without surgery involves a range of methods, each tailored to the individual's specific needs and the underlying cause of the condition.
Assistive Devices |
Foot and ankle specialists often recommend using foot tapings, braces, or shoe inserts (orthoses). These devices aim to correct flexible deformities and offload pressure points, providing support and alleviating discomfort. |
Medication |
Pain and anti-inflammatory medications are often prescribed to provide relief from symptoms. These can help manage pain and reduce swelling. |
Physical Therapy |
Patients can engage in physical therapy to strengthen and stretch the muscles and tendons in the feet. This can improve flexibility, mobility, and overall foot health. |
When non-surgical treatments for adult flatfoot are not effective, surgical intervention may be considered.
Surgical options often involve reconstructive procedures, addressing both soft tissue (tendons, ligaments) and bony corrections. These surgeries aim to repair the underlying bone and tendon problems causing pain and dysfunction.
Schedule An Appointment With Us
Consult our MOH-accredited orthopaedic surgeon for an accurate diagnosis & personalised treatment plan.
While not all cases of adult flatfoot can be prevented, certain measures can help reduce the risk or delay its progression.

MBBS
MRCSEd
MMED (Ortho)
FRCSEd
With over 20 years of experience, Dr Poh Seng Yew is an orthopaedic surgeon specialising in hip, knee, shoulder and elbow surgery, sports medicine, and trauma surgery.




Weekdays: 9.00am – 5.00pm
Saturdays: 9.00am – 1.00pm
Sundays and Public Holidays: Closed
Please leave us a message, and we will be in touch with you shortly.
Exercises focusing on strengthening and stretching the muscles and tendons in the feet can be beneficial. These might include calf stretches, arch lifts, and toe curls. Regular practice of these exercises, along with guidance from a foot and ankle specialist, can improve foot health and alleviate symptoms of flatfoot.
Walking barefoot, particularly on varied surfaces, can help strengthen the muscles in the feet. Balance this with wearing supportive footwear, especially if you are experiencing pain or discomfort. A foot specialist can provide personalised guidance on the best approach for each case.
Untreated adult flatfoot can progress, potentially leading to increased discomfort and further complications in foot function. It can contribute to issues such as ankle problems, knee conditions, lower back pain, and the development of conditions like shin splints and plantar fasciitis. Seek guidance from a foot and ankle specialist for timely treatment and effective management strategies.