Schedule An Appointment With Us
Are Your Symptoms Affecting Your Quality Of Life?
Consult our MOH-accredited frozen shoulder specialist for a comprehensive diagnosis of your condition & a personalised treatment plan.
Frozen shoulder, medically known as adhesive capsulitis, is a condition characterised by stiffness and pain in the shoulder joint.
MBBS
MRCSEd
MMED (Ortho)
FRCSEd

The exact cause of frozen shoulder remains unclear, but the underlying mechanisms are believed to involve inflammation and fibrosis of the joint capsule. Several factors are known to increase its risk:
In some instances, frozen shoulder occurs without any discernible predisposing factors. This leads to its classification into two categories:
The main symptom is a progressive decrease in shoulder joint mobility, accompanied by pain. This pain is usually dull or aching and is typically worsened by movement or at night. This can lead to reduced mobility in the shoulder, making it difficult to perform routine tasks such as dressing, reaching overhead, or even combing hair. It is also not uncommon for the pain and stiffness to cause discomfort in the upper arm.
The condition typically evolves through three stages, with varying degrees of pain and immobility:
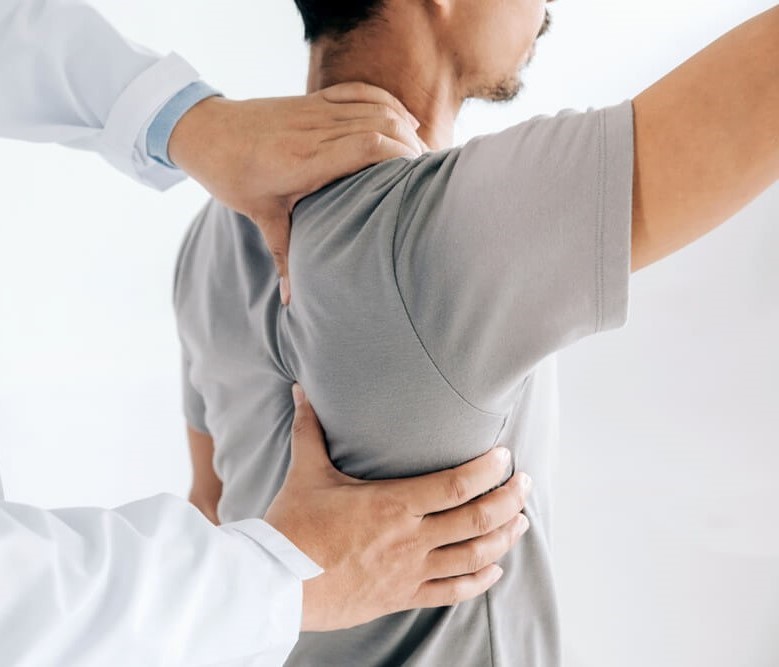
Diagnosing frozen shoulder typically involves a review of symptoms and a physical examination.
Schedule An Appointment With Us
Consult our MOH-accredited frozen shoulder specialist for a comprehensive diagnosis of your condition & a personalised treatment plan.
Non-surgical treatments aim to alleviate pain and restore range of motion.
Surgical intervention for frozen shoulder is considered when non-surgical treatments have not provided sufficient relief.
While it may not be possible to prevent frozen shoulder in every case, certain strategies can reduce the risk or lessen the severity of the condition.

MBBS
MRCSEd
MMED (Ortho)
FRCSEd
With over 20 years of experience, Dr Poh Seng Yew (傅圣耀) is an orthopaedic surgeon specialising in hip, knee, shoulder and elbow surgery, sports medicine, and trauma surgery.




Weekdays: 9.00am – 5.00pm
Saturdays: 9.00am – 1.00pm
Sundays and Public Holidays: Closed
Your symptoms shouldn’t affect your quality of life or disrupt daily activities. Reach out to our friendly clinic staff today & schedule a consultation.
The duration varies, but typically it lasts from 1 to 3 years. The condition goes through three stages: freezing, frozen, and thawing, each varying in length.
While it’s rare for frozen shoulder to recur in the same shoulder, the opposite shoulder can be affected in up to 20% of individuals.
No, surgery is not always necessary. Many cases improve with non-surgical treatments like physical therapy, medication, and home exercises.
Activities that involve heavy lifting or extensive shoulder movements may aggravate the condition. Modify activities to avoid further shoulder strain.
Yes, conditions such as diabetes, thyroid disorders, and certain cardiovascular diseases are associated with a higher risk of developing frozen shoulder.