Schedule An Appointment With Us
Are Your Symptoms Affecting Your Quality Of Life?
Consult our MOH-accredited orthopaedic surgeon for an accurate diagnosis & personalised treatment plan.
MBBS
MRCSEd
MMED (Ortho)
FRCSEd
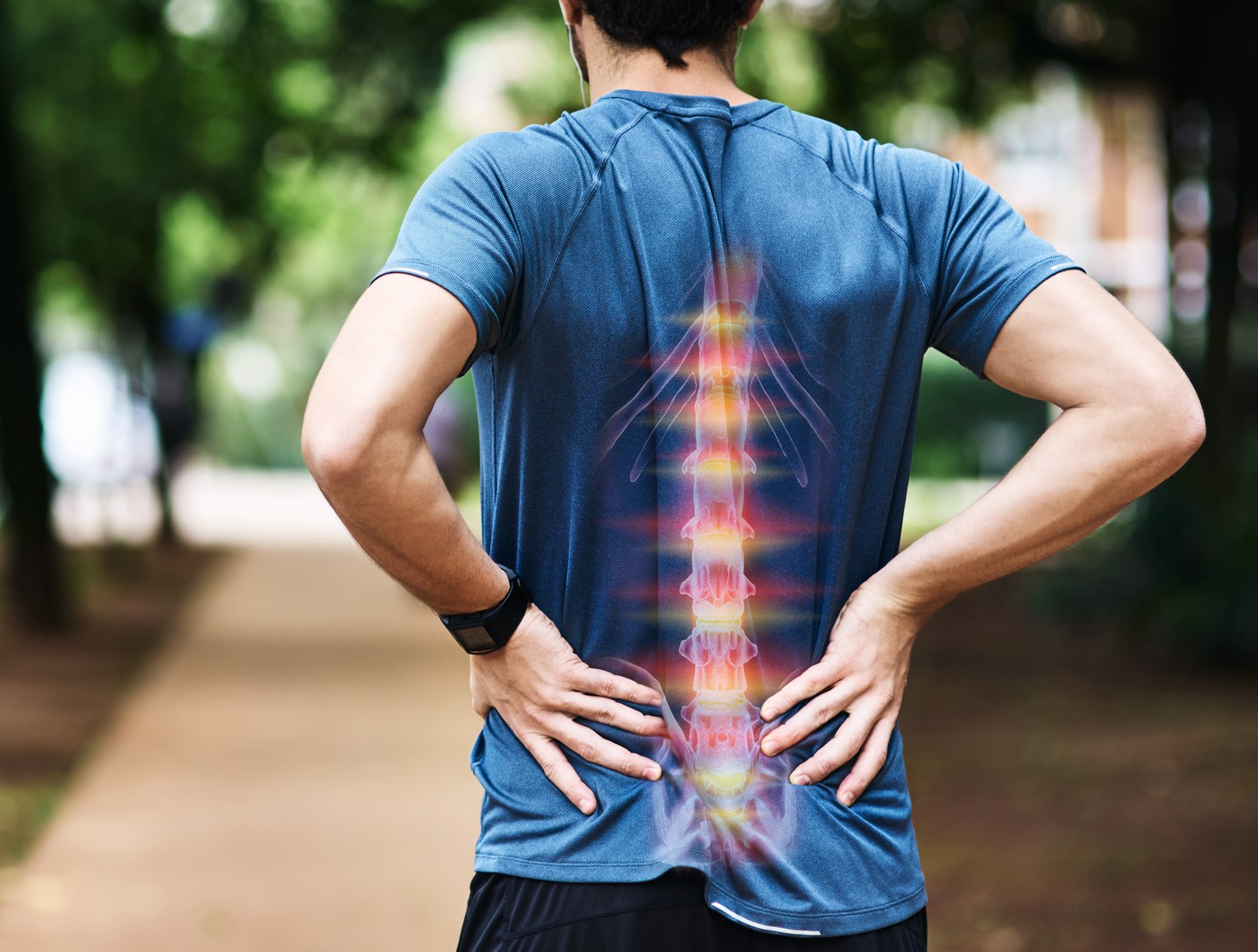
Disc herniation, commonly referred to as a herniated or ruptured disc, is a spinal condition that can lead to discomfort and pain. It involves the intervertebral discs, which are soft, cushion-like structures located between the vertebrae. These discs act as shock absorbers and allow for mobility in the spine.
In disc herniation, the inner, jelly-like material of a disc protrudes through its tougher outer layer, potentially pressing on nearby nerves which causes pain and other symptoms.
The primary cause of disc herniation is the wear and tear of intervertebral discs, often associated with ageing. These discs are needed to maintain spinal flexibility and absorb shocks.
Symptoms of disc herniation vary based on its location and severity. They can include:
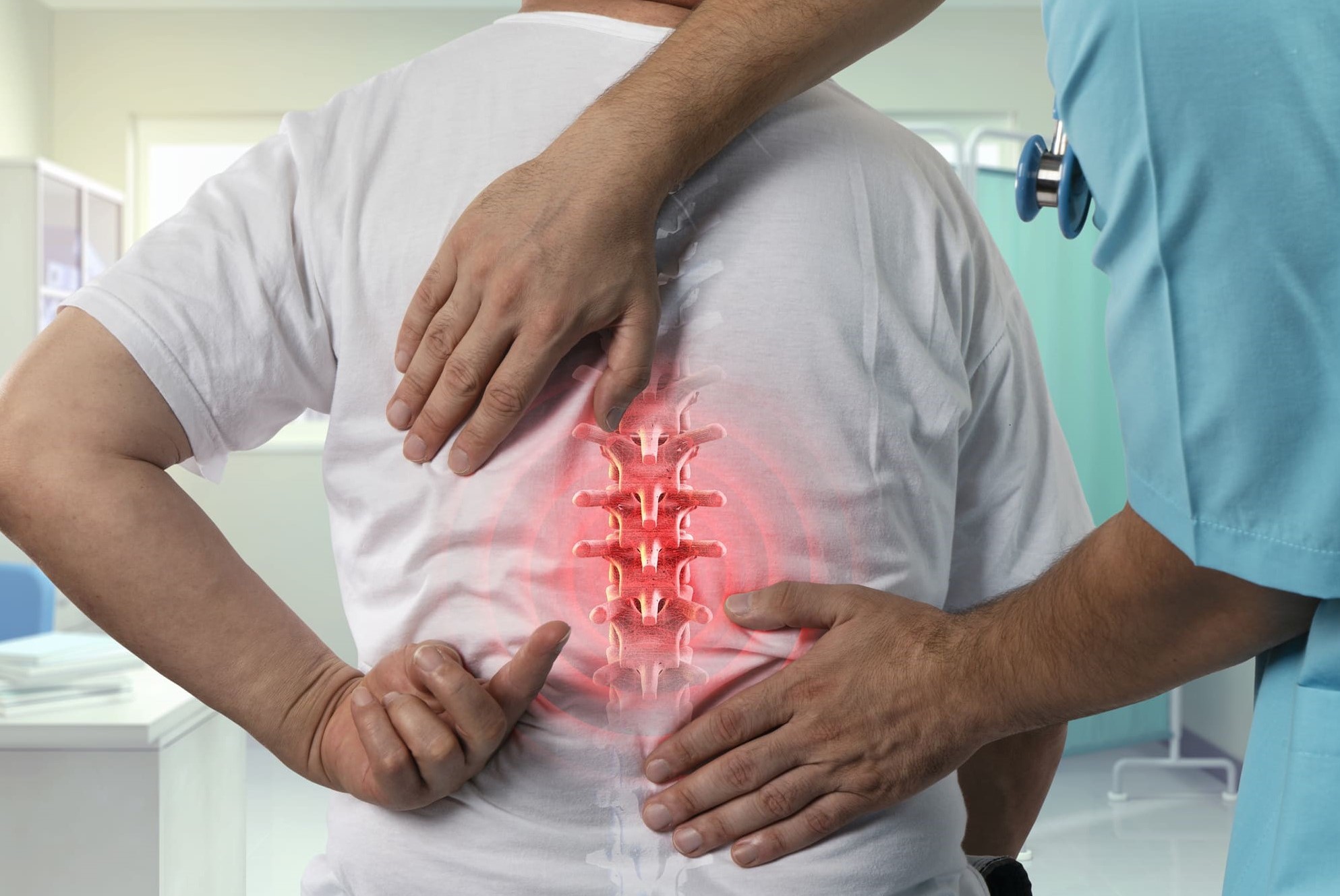
The diagnosis of disc herniation involves several key steps:
Non-surgical methods focus on alleviating pain and improving function in cases of herniated discs.
Rest and Activity Modification |
Initial management suggested by the spine specialist may include rest and reducing activities that aggravate the condition. Patients are educated on proper body mechanics and ergonomic principles to minimise spinal stress, which can help prevent further injury and aid recovery. |
Physical Therapy |
Tailored exercise programs focus on strengthening the muscles supporting the spine. These exercises also aim to improve spinal flexibility and posture, which can help alleviate pain and prevent recurrence. |
Medications |
A range of medications, including non-steroidal anti-inflammatory drugs for reducing inflammation, muscle relaxants to ease muscle spasms, and pain relievers for managing discomfort, can be prescribed. These address various aspects of the pain and inflammation associated with disc herniation. |
Heat and Cold Therapy |
Application of heat or cold packs to the affected area is a simple yet effective method for temporary relief. Heat therapy increases blood flow and relaxes muscles, while cold therapy reduces inflammation and numbs sore tissues. |
Epidural Steroid Injections |
For persistent pain, corticosteroid injections are administered into the epidural space near the affected nerve. This treatment aims to reduce nerve inflammation and pain, providing relief in many cases. |
When non-surgical methods are ineffective or for more serious cases of disc herniation, surgery may be considered.
This procedure targets the specific portion of the herniated disc that compresses the nerve. Minimally invasive techniques can be used to remove this fragment, which often results in rapid pain relief and recovery. It is particularly effective for patients with severe or debilitating pain that has not responded to conservative treatments.
When herniation is accompanied by spinal stenosis (narrowing of the spinal canal), a laminectomy can be performed. This involves removing part of the vertebral bone (lamina) to create more space for the nerves, thereby relieving pressure and pain.
This is considered in cases of severe instability in the spine caused by disc degeneration. By fusing two or more vertebrae, the spine is stabilised and pain can be alleviated. This reduces spinal flexibility and necessitates a longer recovery period.
As an alternative to fusion, this surgery involves replacing the damaged disc with a prosthetic one. This aims to maintain spinal motion, reduce pain, and prevent the degeneration of adjacent segments of the spine, a common complication after fusion surgery.
Schedule An Appointment With Us
Consult our MOH-accredited orthopaedic surgeon for an accurate diagnosis & personalised treatment plan.
Several preventive measures can help reduce the risk of disc herniation.

MBBS
MRCSEd
MMED (Ortho)
FRCSEd
With over 20 years of experience, Dr Poh Seng Yew (傅圣耀) is an orthopaedic surgeon specialising in hip, knee, shoulder and elbow surgery, sports medicine, and trauma surgery.




Weekdays: 9.00am – 5.00pm
Saturdays: 9.00am – 1.00pm
Sundays and Public Holidays: Closed
Please leave us a message, and we will be in touch with you shortly.
While our clinic is located at Mount Elizabeth Novena, our specialists are also able to admit patients and perform surgeries at other private hospitals, including Mount Alvernia Hospital, Farrer Park Hospital, and Thomson Medical Centre.
Accelerating the healing process for a herniated disc involves an integrated approach, including rest, appropriate physical activities, and medications. Engaging in physical therapy that strengthens the back and improves flexibility is beneficial. A spine specialist can offer a personalised treatment plan suited to your specific condition.
Recovery time varies, depending on the severity of the herniation and the chosen treatment approach. While some patients may notice improvement within weeks, others might require months. Consistent follow-up and adherence to the treatment plan can help facilitate recovery.
Managing a herniated disc requires a balanced approach to rest and movement. While rest can initially alleviate acute pain, prolonged inactivity might worsen symptoms. Guided exercises and physical therapy can improve recovery outcomes.
Untreated disc herniation can lead to persistent pain and potential long-term complications. Early assessment and treatment by a spine specialist can help avoid these outcomes and improve quality of life.