Schedule An Appointment With Us
Are Your Symptoms Affecting Your Quality Of Life?
Consult our MOH-accredited hip osteotomy specialist for a comprehensive diagnosis of your condition & a personalised treatment plan.
Hip osteotomy is a surgical procedure predominantly used to treat hip dysplasia.
MBBS
MRCSEd
MMED (Ortho)
FRCSEd
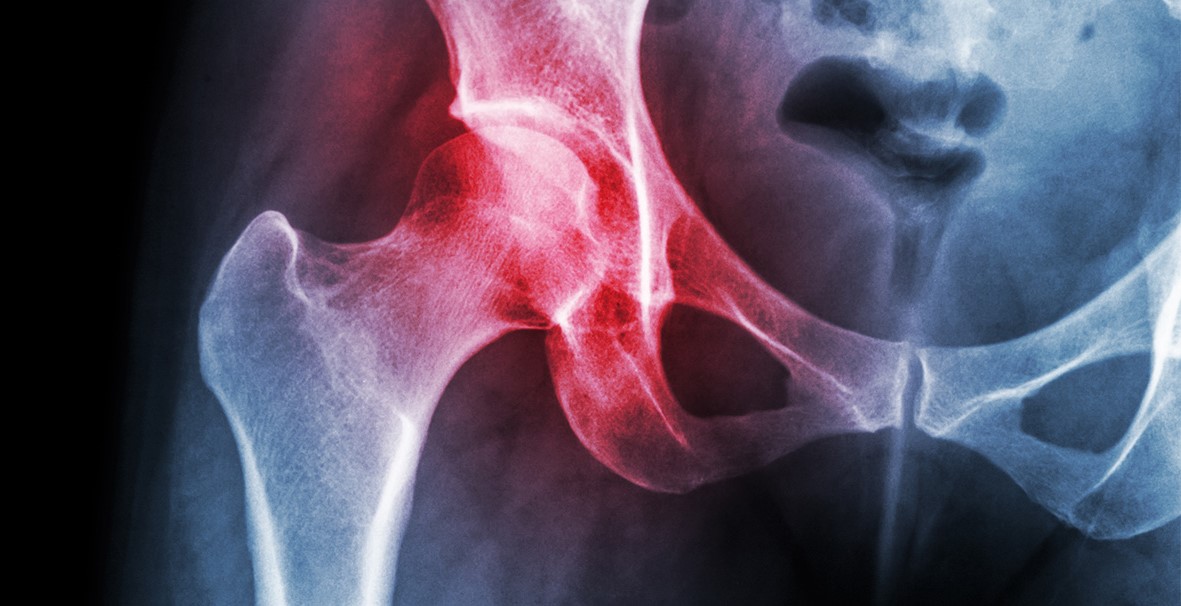
Hip osteotomy is a surgical procedure predominantly used to treat hip dysplasia. This condition arises from a deformity in the acetabulum, the socket part of the hip joint. In hip dysplasia, the acetabulum is not deep enough to securely hold the femoral head, the ball portion of the joint.
During a hip osteotomy, a surgeon reorients the acetabulum over the femoral head. This repositioning aims to provide relief from symptoms and preserve the natural hip joint by improving its alignment and function.
Hip osteotomy is typically considered in the following situations:
The planning phase for a hip osteotomy is comprehensive and typically involves the following:
The hip osteotomy involves a series of carefully executed steps:
In some cases, additional procedures such as a femoral osteotomy may be required to correct misalignment of the femur. Hip arthroscopy might also be performed alongside hip osteotomy to repair damaged labrum or cartilage.
Throughout the procedure, X-ray guidance is used to ensure accurate bone cuts and optimal coverage and alignment of the hip joint.
The procedure usually takes three to four hours.
Hip osteotomy offers several benefits, particularly for individuals with hip dysplasia:
Improved Joint Function |
By realigning the hip joint, the procedure enhances joint function, providing relief from discomfort and improving mobility. |
Preservation of Natural Hip Joint |
The surgery aims to preserve the natural hip joint, which can be preferable to joint replacement, especially in younger patients. |
Reduced Progression of Joint Damage |
By correctly aligning the hip, the surgery slows down the progression of damage to the cartilage and labrum in the hip. This can be particularly beneficial in delaying the onset of arthritis. |
Potential Delay of Hip Replacement |
In many cases, hip osteotomy can delay or even avoid the necessity for a hip replacement later in life. This is especially advantageous for patients who have not yet developed advanced osteoarthritis. |
Schedule An Appointment With Us
Consult our MOH-accredited hip osteotomy specialist for a comprehensive diagnosis of your condition & a personalised treatment plan.
Like any surgical procedure, hip osteotomy carries certain risks and potential complications:
Recovery from a hip osteotomy involves several stages:
Most patients can return to work approximately three months after surgery. Resuming sports activities may take between six to 12 months, depending on individual recovery rates.
The long-term outlook following a hip osteotomy is generally positive, with the procedure improving joint function and quality of life, and potentially delaying the need for hip replacement surgery.

MBBS
MRCSEd
MMED (Ortho)
FRCSEd
With over 20 years of experience, Dr Poh Seng Yew (傅圣耀) is an orthopaedic surgeon specialising in hip, knee, shoulder and elbow surgery, sports medicine, and trauma surgery.




Weekdays: 9.00am – 5.00pm
Saturdays: 9.00am – 1.00pm
Sundays and Public Holidays: Closed
Your symptoms shouldn’t affect your quality of life or disrupt daily activities. Reach out to our friendly clinic staff today & schedule a consultation.
While some discomfort is expected after any surgical procedure, hip osteotomy pain is manageable. Our hip surgeon prioritises pain management, utilising various medications to ease discomfort during the recovery process. Each patient’s experience with pain will vary, but with proper care, it can be effectively controlled.
The longevity of a hip osteotomy depends on various factors, including the patient’s age, activity level, and the specifics of their condition. Generally, the procedure aims to preserve the natural hip joint, potentially delaying the need for a hip replacement for many years.
Post-operative recovery typically involves a balance of rest and gradual mobilisation. Initially, rest can help aid healing, but gentle walking, as recommended by the hip surgeon, can help you regain strength and mobility. We can provide tailored guidance on the appropriate balance between walking and resting during recovery.
Adhering to the prescribed rehabilitation plan and closely following post-surgical instructions provided by the hip surgeon can contribute to a faster recovery. The expertise and guidance of our hip surgeon can help you recover effectively.