Schedule An Appointment With Us
Are Your Symptoms Affecting Your Quality Of Life?
Consult our MOH-accredited knee osteoarthritis specialist for a comprehensive diagnosis of your condition & a personalised treatment plan.
Knee osteoarthritis involves the gradual deterioration of cartilage, which is the cushion which allows for smooth joint movements, in the knee joint. As cartilage thins and wears away, bones within the joint may rub against each other, leading to pain, swelling, and reduced mobility.
MBBS
MRCSEd
MMED (Ortho)
FRCSEd
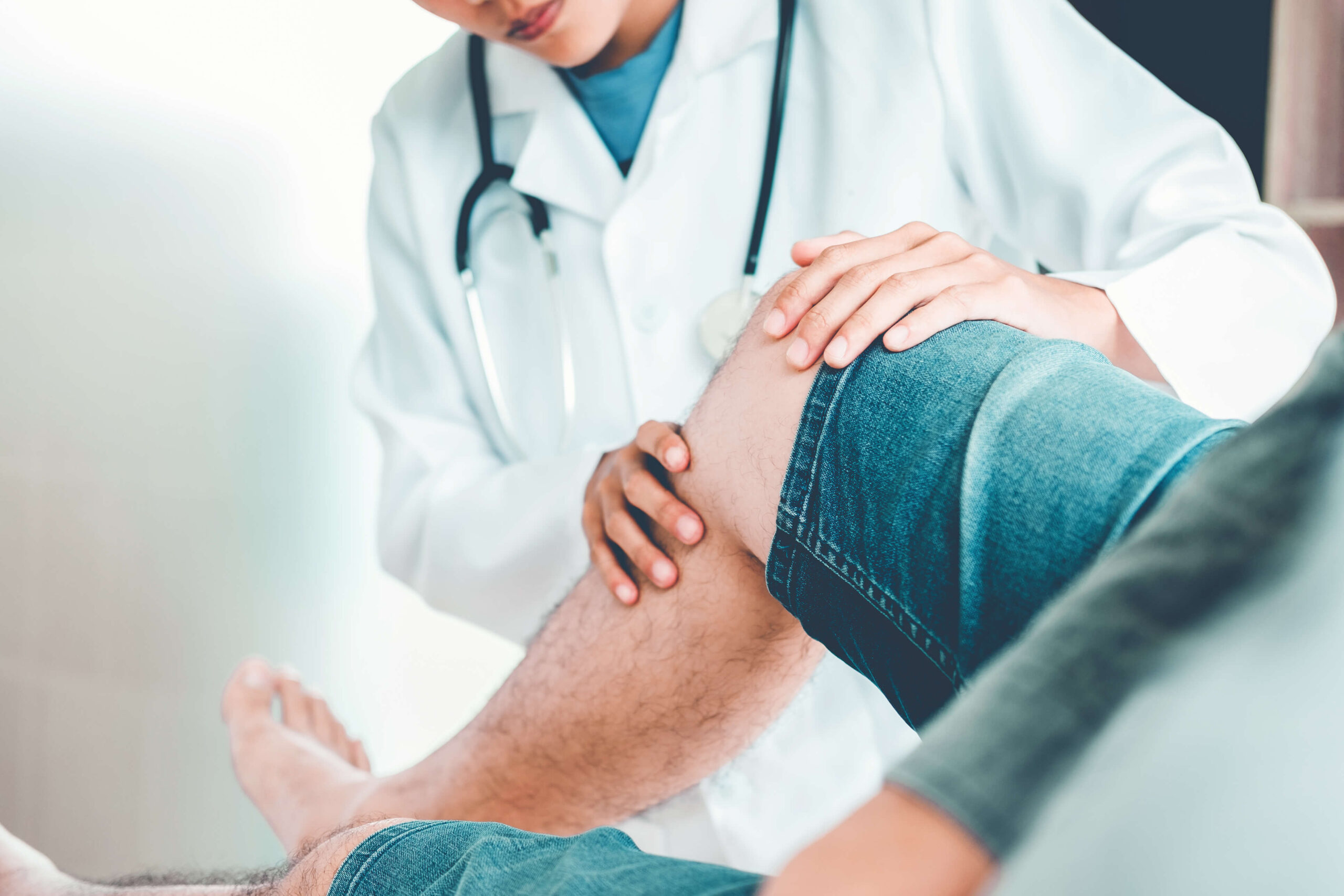
The main factor contributing to knee osteoarthritis is age. As people age, the risk of developing osteoarthritis increases due to the natural wear and tear of joints over time.
Other causes may include:
The symptoms and signs of knee osteoarthritis typically develop gradually and may include:
The diagnosis of knee osteoarthritis typically includes:
Schedule An Appointment With Us
Consult our MOH-accredited knee osteoarthritis specialist for a comprehensive diagnosis of your condition & a personalised treatment plan.
Non-surgical treatments for knee osteoarthritis focus on alleviating symptoms and improving joint function.
In cases where non-surgical treatments do not sufficiently alleviate symptoms of knee osteoarthritis, surgical options may be considered.
While knee osteoarthritis cannot be completely prevented, certain strategies can reduce the risk and slow the progression of the condition.
Schedule An Appointment With Us
Consult our MOH-accredited knee osteoarthritis specialist for a comprehensive diagnosis of your condition & a personalised treatment plan.

MBBS
MRCSEd
MMED (Ortho)
FRCSEd
With over 18 years of experience, Dr Poh Seng Yew is an orthopaedic surgeon specialising in hip, knee, shoulder and elbow surgery, sports medicine, and trauma surgery.




Weekdays: 9.00am – 5.00pm
Saturdays: 9.00am – 1.00pm
Sundays and Public Holidays: Closed
Your symptoms shouldn’t affect your quality of life or disrupt daily activities. Reach out to our friendly clinic staff today & schedule a consultation.
There is currently no cure for knee osteoarthritis. Treatment focuses on managing symptoms and improving joint function.
While age is a risk factor, knee osteoarthritis is not an inevitable part of ageing. Lifestyle choices and preventive measures can influence its development and progression.
Osteoarthritis pain typically worsens with activity and improves with rest. It’s often accompanied by joint stiffness, especially in the morning or after periods of inactivity.
Appropriate exercise, especially low-impact activities, is beneficial. High-impact or strenuous activities might exacerbate the condition.
Complete prevention may not be possible, but risk factors can be managed. Maintaining a healthy weight, regular exercise, and avoiding joint injuries can help.