Robotic-assisted knee replacement uses 3D imaging and computer-guided instruments to map your knee’s unique anatomy before any incision is made. Traditional knee replacement relies on mechanical guides and the surgeon’s visual assessment during the procedure. Both approaches aim to remove damaged cartilage and bone. They then position artificial components to restore knee function. However, they differ significantly in how that positioning is achieved.
The distinction matters because knee replacement success depends heavily on implant alignment. Misalignment by even a few degrees can affect how the weight is distributed across the artificial joint. This potentially influences wear patterns and long-term function. Robotic systems address this by creating a virtual surgical plan based on CT scans (detailed X-ray images from multiple angles) of your specific bone structure. Traditional methods use standardised instruments designed for average anatomy.
How Traditional Knee Replacement Works
Traditional knee replacement follows a systematic approach refined over many decades of orthopaedic practice. The surgeon accesses the knee joint through an incision. They then use mechanical cutting guides—metal jigs positioned against anatomical landmarks—to determine where and at what angle to remove bone.
These guides reference standard anatomical points: the centre of the hip, the centre of the ankle, and specific landmarks on the knee itself. The surgeon aligns instruments based on these references. They make bone cuts with an oscillating saw. They then test how well the trial components fit before implanting the final prosthesis (artificial joint).
Surgeon Experience in Traditional Methods
Traditional surgery places significant emphasis on the surgeon’s tactile feedback and visual assessment. During the procedure, the surgeon evaluates soft tissue tension by manually testing how the knee flexes and extends with trial components in place. Adjustments happen in real-time based on what the surgeon sees and feels.
This hands-on approach means outcomes correlate strongly with surgical volume and experience. Surgeons who perform traditional knee replacements regularly develop refined judgement about bone cuts, ligament balancing, and component sizing that complements the mechanical instrumentation.
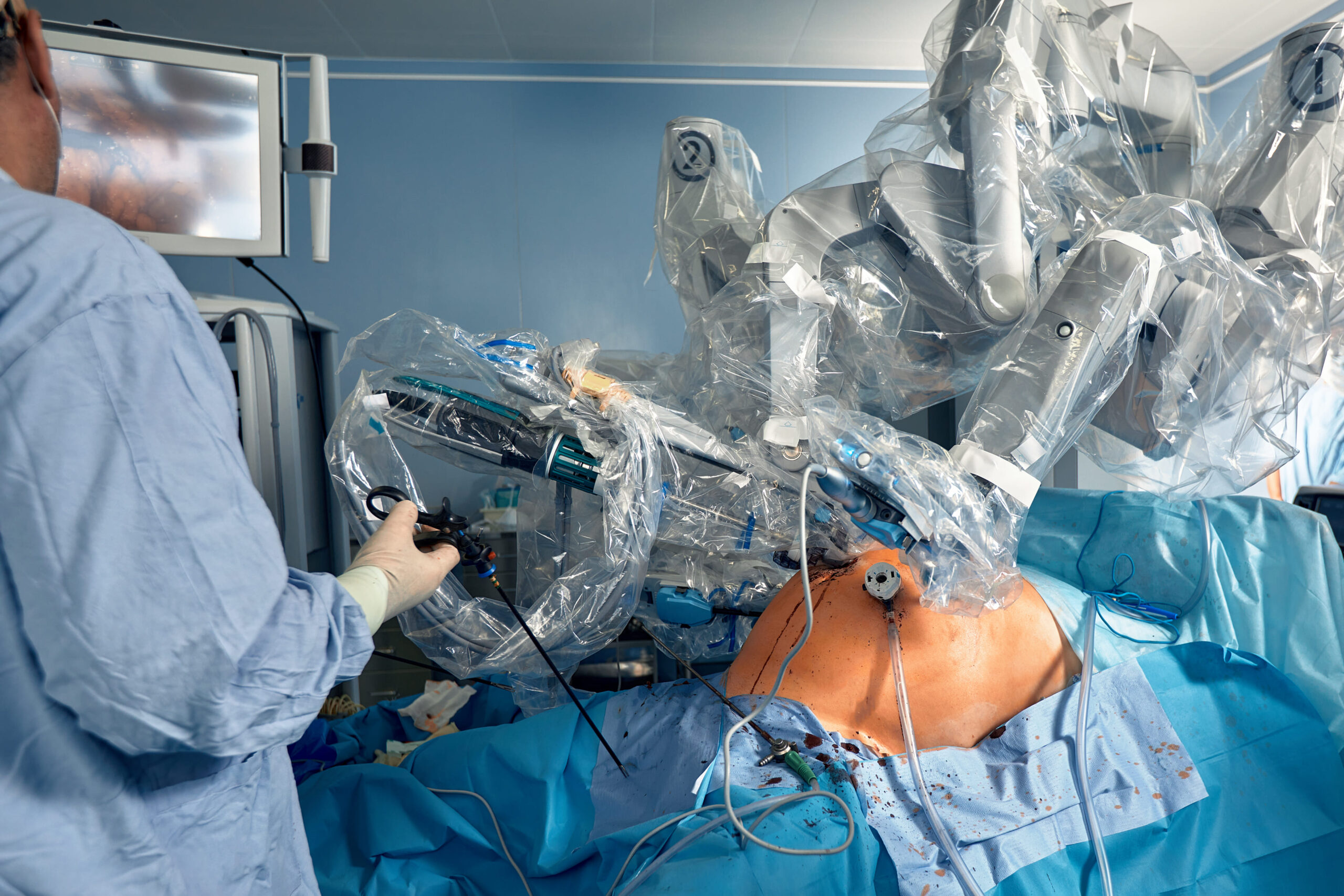
How Robotic-Assisted Knee Replacement Works
Robotic knee surgery adds a preoperative planning phase and intraoperative computer guidance to the surgical process. Before surgery, you undergo a CT scan that creates a detailed 3D model of your hip, knee, and ankle. Software analyses this model to map your bone geometry, joint line position, and alignment.
Using this data, your surgeon plans the procedure virtually—determining exact bone resection depths, angles, and component positions specific to your anatomy. This plan transfers to the robotic system. The system then guides the surgical instruments during the actual operation.
Intraoperative Guidance Mechanisms
During surgery, the robotic arm constrains the cutting instrument to the pre-planned boundaries. If the surgeon moves outside the planned cutting zone, the system either stops the blade or provides haptic feedback (resistance through the handpiece) to indicate deviation.
The surgeon remains in control throughout—the robot doesn’t operate autonomously. Instead, it functions as a precision guide that prevents unintended cuts beyond planned parameters. Real-time tracking cameras monitor the position of instruments and bones. They update the system if the leg shifts during surgery.
Some systems also provide live feedback on ligament tension and joint spacing. This allows surgeons to verify soft tissue balance matches preoperative goals before finalising implant placement.
Precision and Implant Positioning
The measurable difference between approaches appears in implant positioning accuracy. Studies suggest robotic systems achieve planned bone cuts within tighter tolerances than traditional methods, and research documents lower rates of alignment outliers with robotic techniques compared to conventional instrumentation.
However, it is important to note that improved radiographic alignment does not automatically translate into better functional outcomes — multiple systematic reviews have found that clinical results and complication rates remain broadly similar between well-performed robotic and conventional procedures. Your surgeon can explain what this means for your specific situation.
Bone Conservation
Robotic planning allows surgeons to optimise bone cuts for each patient’s anatomy rather than following standardised resection depths. In some cases, this means preserving more healthy bones. This is particularly relevant for younger patients who may eventually need revision surgery.
The CT-based planning also identifies areas of bone loss or defects before surgery begins. Surgeons can plan how to address these issues rather than discovering them mid-procedure.
Soft Tissue Balancing Approaches
Knee replacement success requires more than accurate bone cuts. The ligaments and soft tissues surrounding the joint must be appropriately tensioned. An overly tight knee restricts movement and causes pain. An overly loose knee feels unstable.
Traditional surgery addresses soft tissue balance through the surgeon’s manual assessment. After making bone cuts and inserting trial components, the surgeon flexes and extends the knee. They evaluate how it moves and whether adjustment is needed. Soft tissue releases (small cuts to tight ligaments) may be performed based on this assessment.
Robotic systems quantify this process. Sensors measure the force required to open the joint space at different flexion angles. This provides numerical data about ligament tension. Surgeons can compare these measurements against target ranges. They then adjust bone cuts or soft tissue tension accordingly.
💡 Did You Know?
The ligaments around your knee naturally have different tensions at different bending angles. Balancing a knee replacement means achieving appropriate tension throughout the full range of motion, not just in one position.
Incision Size and Tissue Disruption
Both traditional and robotic approaches can be performed through similar incision lengths. The robotic equipment doesn’t inherently require larger or smaller incisions than traditional instruments.
What differs is the cutting mechanism. Traditional oscillating saws remove bone in the path of the blade. Some robotic systems use burrs (rotating tools that gradually remove bone) that remove bone more gradually and precisely within defined boundaries. This may reduce inadvertent soft tissue contact during bone preparation. However, response times vary depending on your specific condition and the system used.
The surgical approach—how muscles and tendons are managed to access the joint—affects recovery more than whether robotic assistance is used. Surgeons using either method can employ tissue-sparing techniques.
Operating Time Considerations
Robotic procedures may take longer than traditional knee replacements in many cases, particularly earlier in a surgeon’s experience with the system. A 2023 study examining six randomised clinical trials across 1,689 cases found that robotic-assisted surgery was associated with a longer operating duration, with a mean difference of around 32.9 minutes. A large 2025 study from an Asian public healthcare system reported mean surgical times approximately 20.6 minutes longer for robotic procedures. Research also indicates that as surgeons gain experience — typically after 30 to 40 robotic procedures — operative times tend to approach those of manual surgery.
The additional time comes from system setup, registration, and the bone preparation process. For straightforward cases performed by experienced teams, this difference may be modest. Complex cases involving significant deformity or prior surgery may see larger variations.
Recovery and Rehabilitation Factors
Recovery from knee replacement depends on multiple factors: your preoperative function, overall health, pain management, and rehabilitation engagement. The surgical approach—robotic or traditional—represents one variable among many.
Some studies report that patients with robotically placed implants may experience shorter hospital stays and earlier home discharge, though differences in daily rehabilitation milestones are less consistently observed across the research. Individual recovery depends far more on the factors listed below.
- Preoperative knee range of motion and muscle strength
- Body weight and overall conditioning
- Pain control effectiveness
- Physiotherapy compliance and quality
- Presence of other joint problems affecting mobility
⚠️ Important Note
Neither surgical method eliminates the need for dedicated rehabilitation. Achieving full benefit from knee replacement requires consistent physiotherapy regardless of the surgical technique used.
Suitability and Selection Factors
Not every patient requires robotic assistance. Not every surgeon offers it. The decision involves weighing potential precision benefits against practical considerations including availability, cost, and surgical team experience. Your doctor will determine which approach is most suitable based on your specific anatomy, condition severity, and individual risk factors.
Robotic surgery may offer particular advantages for:
- Patients with unusual anatomy or significant deformity
- Younger patients where bone conservation matters for future revision options
- Partial knee replacements (where only damaged portions are replaced) where preserving healthy compartments requires precise boundaries
- Patients with prior knee surgery affecting standard anatomical landmarks
Traditional surgery remains appropriate for many patients, particularly those with straightforward anatomy and access to experienced high-volume surgeons. The technique has documented long-term success across many procedures.
Questions to Discuss with Your Surgeon
When evaluating surgical options, specific questions help clarify what’s most relevant for your situation:
About your anatomy: Does imaging show any unusual bone shape, prior injury, or deformity that affects surgical planning? How would each approach address these factors?
About surgeon experience: How many knee replacements does the surgeon perform annually? For robotic cases, what is their specific experience with that system?
About expected outcomes: Based on your condition, what range of motion and function is realistic? How do outcomes compare between approaches in the surgeon’s own practice?
About logistics: What is the preoperative process for each approach? How do hospital stays and early recovery protocols differ?
When to Seek Professional Help
Consider orthopaedic evaluation if you experience:
- Knee pain limiting daily activities like walking or climbing stairs
- Knee stiffness that doesn’t improve with movement
- Pain that persists despite anti-inflammatory medications and physiotherapy
- Knee swelling that recurs or doesn’t resolve
- Difficulty with activities you previously managed comfortably
- Night pain disrupting sleep
- Knee instability or giving way episodes
Commonly Asked Questions
Does robotic surgery guarantee a better outcome than traditional surgery?
No surgical method guarantees specific outcomes. Robotic assistance improves precision in implant positioning. However, successful knee replacement depends on appropriate patient selection, surgical execution, implant quality, and postoperative rehabilitation. A well-performed traditional surgery by an experienced surgeon can achieve comparable results to robotic surgery.
Is the robot performing my surgery?
The surgeon performs the surgery while the robotic system provides guidance. The robot constrains instruments to pre-planned boundaries. However, it doesn’t make decisions or operate independently. Your surgeon controls all aspects of the procedure.
Will I need a CT scan before robotic surgery?
Most robotic knee replacement systems require preoperative CT imaging to create the 3D surgical plan. This scan involves radiation exposure and an additional appointment before surgery. Some newer systems use different imaging or intraoperative registration methods.
Does robotic surgery cost more?
Robotic systems involve significant capital and maintenance costs that may affect surgical fees or hospital charges. Discuss costs directly with your surgical team and clarify what’s included in quoted fees.
How do I know which approach is right for me?
Consultation with an orthopaedic surgeon who offers both approaches provides a balanced perspective for your individual situation. This decision involves your specific anatomy, condition severity, functional goals, surgeon recommendation, and practical factors like availability and cost.
Important Disclaimer: Outcomes differ among patients based on individual health factors including anatomy, overall health status, adherence to rehabilitation protocols, and other personal variables. The information provided here is educational and should not replace personalised medical advice from your healthcare provider. Always consult with qualified healthcare professionals to discuss your specific situation and determine the most appropriate treatment approach for your needs.
Next Steps
Both robotic and traditional knee replacement can effectively address knee arthritis when appropriately matched to patient needs. Implant alignment is the central variable—robotic systems offer greater precision and individualised planning, while traditional surgery relies on standardised guides and surgeon experience. The appropriate choice depends on your specific anatomy, the presence of deformity or prior surgery, and the surgeon’s experience with each technique. A consultation that includes imaging review and physical examination of your knee is the necessary next step to determine which approach suits your situation.
If you are experiencing knee pain that limits walking or climbing stairs, recurring knee swelling, instability, or night pain, consult with an orthopaedic surgeon to evaluate whether traditional or robotic-assisted knee replacement is appropriate for your condition.